Obsessive-compulsive disorder (OCD) can be debilitating, and exhausting, and greatly reduce the quality of life. While psychotherapy and pharmaceuticals are available as forms of treatment for OCD, a great number of people suffer regardless of their ability to reduce symptoms, don’t respond to these treatment options, or suffer their side effects.
- What Is Obsessive Compulsive Disorder Ocd
- Ocd Symptoms
- Obsessive Signs
- Compulsive Behavior Symptoms
- Ocd And Major Depressive Disorder
- Traditional Treatments For Obsessive Compulsive Disorder
- Exposure And Response Prevention Therapy
- Cognitive Behavioral Therapy Cbt
- Pharmacology
- What Is Transcranial Magnetic Stimulation
- Types Of Tms
- Tms For Ocd
- What Does Dtms Treatment For Ocd Look Like
- Advantages Of Tms For Ocd
- Where Can I Find Tms For Ocd
Luckily, there are new promising alternative treatments available. If you or a loved one is struggling with OCD, transcranial magnetic stimulation (TMS) may be your solution.
What Is Obsessive-Compulsive Disorder (OCD)?
Obsessive-compulsive disorder is one of the mental health conditions that come with severe anxiety. Uncontrollable obsessions in this anxiety disorder lead to compulsive behaviors.
Unreasonable fears, worries, or thoughts come in the form of unwanted, disturbing images or intrusive thoughts, ideas, feelings, or sensations. Frequently occurring, these factors drive those suffering from OCD to carry out rituals and repetitive or compulsive behavior, in an attempt to prevent or get rid of obsessive thoughts and as a way to manage or reduce anxiety.
OCD can be time-consuming and tiring, and create significant distress for a person facing it, as well as take a toll on loved ones and colleagues. With symptom severity ranging from mild to very severe, bettering or worsening, and sometimes coming and going over time, treatment for OCD is vital.
OCD Symptoms

The symptoms of OCD are seen in the obsessive element as well as in the compulsive element.
Obsessive Signs
An underlying theme typically outlines obsessive symptoms. It typically includes difficulty with uncertainty, needing things to be perfectly symmetrical or perfectly in order, thoughts about the loss of control, or sometimes harming oneself or others, aggressive thoughts, a fear of contamination or dirt, or unwanted thoughts on religious or sexual subjects.
A person may experience a fear of touching others or being touched by them. They may feel uncomfortable touching objects that others have touched. If objects are not placed in an orderly way or are not facing a certain direction, they may experience stress or anxiety.
They may excessively worry, particularly about something bad possibly happening, or have a strong need to know things that may be considered trivial. Doubting whether they locked the door or switched off the stove is also a sign. OCD symptoms may come in the form of unpleasant images, or thoughts about acting inappropriately, such as shouting obscenities or driving a car into a crowd of people.
Compulsive Behavior Symptoms
Some behavioral symptoms of OCD are related to body-focused repetitive behavior. These include picking the skin, repeating hand washing to the point that the skin is raw, or hair-pulling. Other compulsive behaviors include arranging things systematically or facing the same way.
A person suffering from OCD may consistently check on their doubts, such as whether they locked the door or switched off the stove, or may pay excessive attention to detail. They could avoid anything that could trigger their compulsions, like shaking another person’s hand. They may engage in hoarding, aggressive impulses, silently repeat words or phrases or count in specific patterns.
OCD and Major Depressive Disorder
Risk factors for developing OCD include genetics, temperament, critical life events, environmental factors, and a history of anxiety disorders or depression. Those suffering from OCD are at risk of developing other mental health disorders. The comorbidity of OCD with major depressive disorder is common, affecting more than one-third of OCD sufferers.
This comorbidity makes life even harder for a person with OCD, as it not only decreases their daily functioning but also causes a poorer response to OCD treatment. Those suffering from the co-occurrence are more likely to experience other anxiety disorders, such as separation anxiety disorder or social phobia.
The presence of major depressive disorder is also linked to more severe OCD symptoms than found in those who are non-depressed OCD sufferers, to the point of increasing the chances of suicide.
Antidepressants are often used to treat both depression and OCD, but in some cases, people are resistant to the medication.
Traditional Treatments for Obsessive-Compulsive Disorder
The traditionally known effective treatments for OCD include exposure and response prevention therapy (ERP), cognitive behavioral therapy, and pharmaceuticals.
exposure and response prevention therapy
ERP works under the guidance of a therapist in a safe environment, whereby a person is gradually exposed to situations that provoke their obsessions. ERP is an OCD treatment that practices confronting obsessions, objects, images, thoughts, or situations that provoke anxiety through exposure. The response prevention element of it aims to get the person to choose not to engage in compulsive behaviors once these obsessions have been provoked.
But since motivation and a willingness to follow through on the consistent practice of ERP, both in therapy sessions and as homework, is needed, depression interferes with this most effective OCD treatment. A decreased interest, motivation, and energy get in the way of consistency, which is why the typical approach is to address depression through the use of medication and cognitive behavior therapy.
cognitive behavioral therapy (CBT)
CBT is a form of psychotherapy that focuses on the thoughts and feelings, as well as on the physical reaction or behavior of OCD patients. It helps people to become less anxious in their reaction to them, while a subtype of CBT, called Acceptance and Commitment Therapy (ACT) helps patients to develop flexibility and openness when reacting to obsessive thoughts, while simultaneously committing to a change in behavior.
pharmacology
Some of the medications used to treat depression are used to treat OCD, too. It is considered one of the treatment options for reducing OCD symptoms, and although effective, remission is uncommon, and many people continue to have symptom severity high enough to still qualify for an OCD diagnosis. Some studies have estimated a significant 30% to 40% of patients remain symptomatic after treatment.
OCD treatment using pharmaceuticals also comes with these medications’ side effects.
What Is Transcranial Magnetic Stimulation?
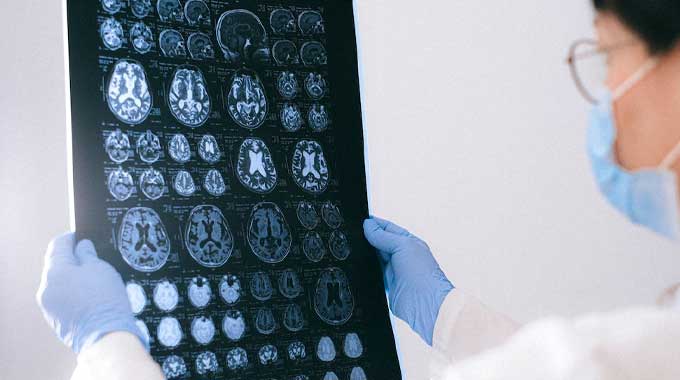
Transcranial magnetic stimulation (TMS) is a non-invasive treatment in the form of brain stimulation, that uses electromagnetic pulses. An electric current that flows through a coil, placed over a person’s head, produces magnetic fields, which pass through the skull and produce a field of electricity underneath it.
Neurons in the brain communicate and connect through brain cells, known as neurotransmitters, and form a neural network when they work together. Brief and repetitive magnetic pulses in TMS therapy reach frontal brain structures and networks, stimulating and exciting underactive brain cells in those who live with various mental health disorders. The stimulation results in altered communication and connectivity between neurons, and an alteration of the neural pathways.
The United States Federal Government approved Transcranial Magnetic Stimulation (TMS) devices for treatment in psychotherapy in 2008, and the treatment was first approved for the treatment of major depression, especially treatment-resistant depression.
By 2018, the Food and Drug Administration (FDA) approved TMS as an alternative treatment for OCD. Researchers and clinicians have also seen its potential success with insomnia, post-traumatic stress disorder, and panic disorder.
Types of TMS
Typically used in treating depression, repetitive transcranial magnetic stimulation (rTMS) treatment is a therapeutic intervention that helps relieve symptom severity, especially in patients that failed to respond to pharmacological treatment options. Repetitive TMS has been shown to change neuron activity in the prefrontal cortex of the brain.
Using a different coil, deep TMS therapy works with a bigger pulse range than standard TMS, targeting both the left and right dorsolateral prefrontal cortex. In this way, deep TMS has a wider range than conventional TMS, and as such can reach deeper structures of the brain directly, such as the limbic system.
That makes deep transcranial magnetic stimulation (dTMS) more effective in treating OCD, treatment-resistant depression, and a wide range of mental health disorders. It is the first new therapy in over a decade to be FDA-cleared to treat OCD.
TMS for OCD

The treatment of obsessive-compulsive disorder is typically carried out with medication, such as selective serotonin reuptake inhibitors (SSRIs), ERP, or a combination of the two.
But with almost one-half of OCD patients failing to respond to their first tried treatment, deep TMS offers a lot.
Particularly vital for those who have not achieved sufficient improvement, a trial that led to FDA clearance of TMS for treating OCD showed its highly effective ability to reduce OCD symptom severity. The randomized control trial showed that, by regulating the neural activity in brain structures associated with OCD, such as the anterior cingulate cortex and medial prefrontal cortex, high-frequency dTMS can improve OCD symptoms.
The primary outcome measure in clinical trials is called the Yale-Brown Obsessive-Compulsive Scale (YBOCS), by which a higher score indicates higher symptom severity. In the trial, the active group achieved a greater reduction in the YBOCS score than the sham group, while a one-month follow-up showed response rates of 45.2% in the dTMS group versus 17.8% in the sham group.
Deep Transcranial Magnetic Stimulation can reduce OCD symptoms by increasing a person’s ability to resist compulsions, while also helping them to engage more effectively with ERP therapy.
It is not only this clinical trial data that is promising. Data collected and published in the Journal of Psychiatric Research in 2020 from 22 clinical sites, including treatment details and outcome measures, showed its benefit in both studies and clinical practice. The majority of OCD patients benefited from deep TMS therapy, evident within 20 sessions. With further treatment, beyond 29 sessions, the results showed a continued reduction of OCD symptoms.
In the very common case where OCD comorbid depression occurs, rTMS has shown to be a positive therapeutic tool. A study showed that 36 repetitive transcranial magnetic stimulation sessions resulted in a full OCD and depression symptom response in most patients.
What Does dTMS Treatment for OCD Look Like?
Before a TMS session, a doctor will review a person’s medical history and recommend the treatment.
A deep TMS session itself is safe, noninvasive, and follows a few simple steps. First, a TMS technician will take measurements to ensure the correct coil positioning over the patient’s head and the patient’s motor threshold is tested.
The initial part of each treatment session will involve a brief, personalized provocation or exposure, whereby the patient is intentionally exposed to their OCD fears, to activate the relevant areas of the brain. This ‘exposure’, specifically designed for each patient, is followed by an 18-minute dTMS treatment session.
The H-Coil will then send a magnetic pulse that acts to regulate the brain’s neural activity as stimulation begins, and a person may experience a tapping sensation underneath the coil. The area that is specifically targeted to treat OCD is called the supplementary motor cortex (SMA), as an overactive SMA is associated with triggered intrusive thoughts and repetitive movements.
In cases where targeting the SMA in OCD treatment is not very effective, other possible locations are considered, such as the orbitofrontal cortex (OFC), the dorsolateral prefrontal cortex (dlPFC), and the anterior cingulate cortex (ACC). After waiting for the therapy to finish, a person goes about their day and can continue normal daily activities, including driving.
Deep TMS typically involves daily treatment, five days per week, for four to six weeks.
Advantages of TMS for OCD
The biggest advantage of TMS treatment is for those who struggle with treatment resistance or those who have had only minimal relief from pharmacological treatment.
TMS for the treatment of obsessive-compulsive disorder shares advantages with its treatment for depression; the many patients who have tried first-line treatments, like ERP, cognitive behavior therapy, and medication, and are still struggling with OCD and/or depression now have an alternative route. Patients treated with dTMS can function at a significantly higher level, without any adverse effects, and in some cases improve faster than with pharmacological approaches.
While deep brain stimulation or psychosurgery has been used as a treatment option for treatment-resistant patients, dTMS treatment comes with less risk, fewer costs, and avoidance of the possible complications that come with these procedures.
Deep TMS does not require sedation or anesthesia. Brain surgery also comes with a particularly anxiety-provoking element for anyone with severe OCD, often causing an unwillingness to proceed. TMS is a noninvasive treatment alternative.
Unlike selective serotonin reuptake inhibitors (SSRIs), dTMS treatment specifically targets brain regions that play a role in regulating symptoms of OCD. This means that the rest of the body is spared side effects common with antidepressant medications. Instead of nausea, sedation, dry mouth, weight gain, or sexual dysfunction, a person may only have to undergo mild discomfort as a TMS treatment side effect, which fades away as therapy continues.
These discomforts include mild headache, a tapping sensation in the scalp, tingling of facial muscles, or redness at the site of stimulation. Deep transcranial magnetic stimulation also does not cause withdrawal when discontinuing therapy, unlike medications.
Without requiring hospitalization, TMS treatment is provided in an office setting. It is also done on an outpatient basis and without cognitive adverse effects, which means that a person can come for treatment early in the morning, between meetings or classes, or on a lunch break. This flexibility makes treatment much more accessible for many patients, and also allows them to receive help without giving up responsibilities outside of treatment.
Deep TMS therapy boosts the effects of exposure and response prevention therapy and does not disregard this cornerstone of OCD treatment. In fact, dTMS can be done alongside ERP and cognitive behavioral therapy, or medications.
Where Can I Find TMS for OCD?
If you or a loved one wants to take back control of your life in the face of mental illness, GIA Chicago can help. As a mental health clinic specializing in transcranial magnetic stimulation, we provide the most cutting-edge and up-to-date evidence-based therapy techniques for OCD.
We custom design a treatment program according to your specific needs. GIA Chicago’s comprehensive admissions procedure and unique set of scientifically validated diagnostic tests allow us to understand your individual mental, physical and health needs, which informs our therapy so that you may get the best care possible.
We believe the road to mental wellness is unique for each person, and that most people respond best to the combination of evidence-based therapies and personal support and attention. Our caring and compassionate staff supports you all the way through your treatment.
With experience in treating a wide range of mental health issues, including depression, anxiety, OCD, and post-traumatic stress disorder, GIA Chicago optimizes a wide range of therapeutic approaches that enhance and promote life-long wellness. Contact us to find out more about our treatment for obsessive-compulsive disorder.





